Understanding Pelvic Organ Prolapse: Causes, Symptoms, and Treatment Options
Imagine stepping into the shower and noticing a feeling of heaviness or pressure in your pelvis. Maybe it feels like something is lower than usual. You might reach down and feel a bulge—or a ball-like sensation.
For many women, this moment is frightening.
Thoughts like “Am I imagining this?”, “Is something seriously wrong?”, or “Could this be cancer?” are very common. Those reactions make sense.
But here’s something important to know:
You’re not imagining it.
And you’re not alone.
What you may be experiencing is pelvic organ prolapse—a common and treatable condition, especially after childbirth. Understanding what’s happening in your body is the first step toward feeling calmer and more in control.
What Is Pelvic Organ Prolapse?
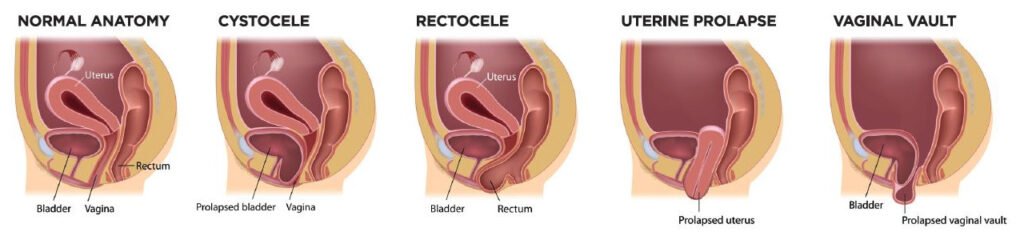
Pelvic organ prolapse occurs when one or more pelvic organs—such as the bladder, uterus, rectum, or intestines—shift downward and press into the vaginal canal.
This happens when the pelvic floor muscles and connective tissues that support these organs become stretched or weakened.
A helpful way to think about prolapse is as a type of hernia.
Just as an abdominal hernia occurs when tissue pushes through a weakened area of the abdominal wall, pelvic organ prolapse occurs when the pelvic floor no longer provides enough support to hold the organs in their usual position.
This condition is more common than many women realize. Research suggests that up to half of women who have had a vaginal delivery will experience some degree of prolapse during their lifetime.
While prolapse can feel uncomfortable or alarming, it is not dangerous, and it is very treatable. Both non-surgical and surgical options are available to improve symptoms and quality of life.
A Patient Story: Putting the Experience Into Words
Many women struggle to describe what prolapse feels like.
One patient, Susie, noticed symptoms after the birth of her third child. She felt heaviness and pressure, and it seemed as though a tampon wouldn’t stay in place—no matter what she tried.
When she came in for an evaluation, she was diagnosed with stage three pelvic organ prolapse. The diagnosis felt overwhelming at first. But once she understood her options, everything shifted.
With appropriate treatment, Susie was able to return to daily life without discomfort or embarrassment.
Stories like hers matter. They remind us that prolapse is not a sign of failure or something being “wrong” with your body.
It’s a medical condition.
And it’s manageable.
Why Does Pelvic Organ Prolapse Happen?
The pelvic floor forms the base of the torso. It’s made up of muscles, ligaments, and connective tissue that support the pelvic organs.
When these tissues weaken, they can no longer hold the organs in place.
Several factors can contribute to this weakening, including:
Pregnancy and childbirth
Trauma during delivery
Aging and hormonal changes, especially during menopause
Chronic constipation or chronic coughing
Excess weight
Genetic predisposition or connective tissue differences
Smoking, which affects tissue health and often increases coughing
Think of the pelvic floor like a trampoline.
When it’s firm and resilient, everything stays supported. When it becomes stretched or weakened, the organs begin to descend—leading to the symptoms of prolapse.
Symptoms of Pelvic Organ Prolapse
Symptoms vary depending on which organs are involved and how advanced the prolapse is. Common signs include:
A feeling of heaviness or pressure in the pelvis
A bulge or ball-like sensation in the vaginal area
Difficulty using tampons
Discomfort during physical activity
Changes in bladder or bowel function
Discomfort during intimacy
Pelvic organ prolapse is not life-threatening.
But it can affect comfort, confidence, and daily life—and that matters.
Non-Surgical Treatment Options
Many women can manage prolapse symptoms without surgery.
Common non-surgical options include:
Pelvic floor physical therapy
Targeted exercises help strengthen the muscles that support the pelvic organs and improve coordination.
Lifestyle adjustments
Addressing factors like constipation, chronic coughing, excess weight, and smoking can reduce strain on the pelvic floor.
Pessary use
A pessary is a soft, silicone device placed in the vagina to support the prolapsed organs. It doesn’t cure prolapse, but it can significantly improve comfort and daily function. Pessaries come in many shapes and sizes, and proper fitting is key.
Surgical Treatment Options
When symptoms persist despite conservative care, surgery may be recommended.
Surgical options depend on which organs are affected and the severity of prolapse. They may include:
Vaginal, laparoscopic, or robotic procedures
Hysterectomy in certain cases
Repair using native tissue or synthetic mesh, when appropriate
A consultation with a fellowship-trained urogynecologist is essential. Surgery should always be individualized, with a clear discussion of risks, benefits, and alternatives.
Living With Pelvic Organ Prolapse
Pelvic organ prolapse is common.
And it is treatable.
Seeking care provides clarity, personalized options, and relief. Whether treatment involves physical therapy, lifestyle changes, a pessary, or surgery, support is available.
If you’re experiencing heaviness, pressure, or bulging:
You are not alone
You are not broken
And you have options
Pelvic floor symptoms can feel isolating but they don’t have to be faced in silence. With the right care, many women return to comfortable, active, and fulfilling lives.
If this message resonated with you, feel free to share it with a friend, sister, or mother who may benefit from understanding her body a little better too. For additional guidance, tips, and exercises focused on pelvic health, follow Dr. Nabila Noor on YouTube, Instagram, and TikTok. Prioritizing your pelvic floor today ensures a healthier, stronger, and more resilient body tomorrow.