Overactive Bladder Syndrome: Understanding Why You Are Always Running to the Bathroom
Do you find yourself constantly looking for the nearest bathroom?
Planning outings around restroom access?
Waking up multiple times each night just to urinate?
If this sounds familiar, you may have been told—or assumed—that you simply have a “small bladder.”
In reality, these symptoms are often caused by a condition called overactive bladder syndrome.
Overactive bladder is common, disruptive, and frequently misunderstood. Many women live with it quietly, believing it’s just part of aging or something they have to tolerate. But that’s not true.
This condition is highly treatable.
And no one needs to live their life around bathroom breaks.
A Patient Story That Reflects a Common Experience
One patient, Reena, came to the office feeling exhausted and overwhelmed. She was running to the bathroom every thirty minutes, which made working as a nurse incredibly challenging. Nights were no better—she was waking up multiple times to urinate.
She assumed her bladder was small.
She thought nothing could be done.
Over time, the emotional impact grew. Her children joked about how often she needed the bathroom. She began avoiding activities she once enjoyed, worried she wouldn’t make it in time.
After a thorough evaluation, Reena was diagnosed with overactive bladder syndrome.
Understanding what was happening—and learning that effective treatment options existed—changed everything. With the right care, she was able to regain comfort, confidence, and control.
What Is Overactive Bladder Syndrome?
Overactive bladder syndrome isn’t a single disease. It’s a group of urinary symptoms that occur together, including:
Urinary urgency – a sudden, intense need to urinate that’s difficult to ignore
Increased frequency – going to the bathroom more often than usual
Nocturia – waking up at night to urinate more than once
Urgency-related leakage – urine loss associated with a strong urge
These symptoms are not caused by laziness or a weak bladder.
They’re often the result of miscommunication between the bladder and the brain.
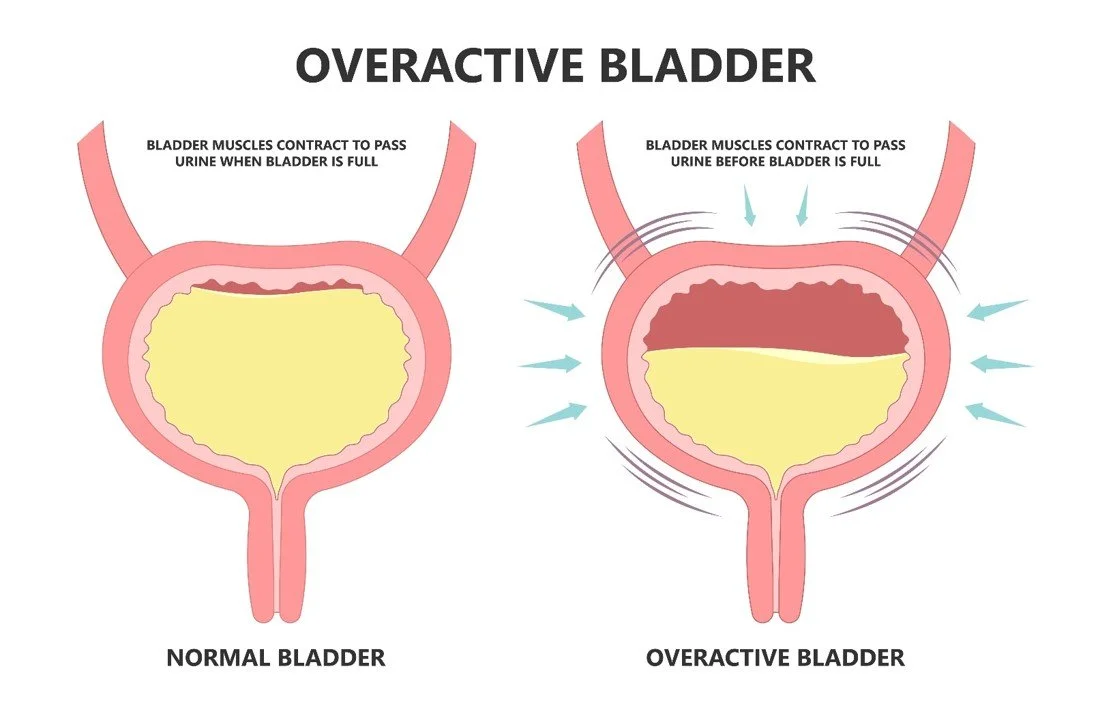
Image by China Medical Universty Hospital
How the Bladder Normally Works
In a healthy system, the bladder functions like a flexible balloon.
As urine fills the bladder, the muscular wall—called the detrusor muscle—gradually stretches. Most women can comfortably hold about 400 to 600 milliliters of urine before the bladder reaches capacity.
At that point:
The bladder contracts
The brain receives the signal that it’s time to urinate
The pelvic floor relaxes
The urethra opens
The bladder empties fully and smoothly
This coordination allows for controlled, predictable urination.
What Changes in Overactive Bladder Syndrome
With overactive bladder, that coordination becomes disrupted.
The detrusor muscle may contract unpredictably—even when the bladder isn’t full. These involuntary contractions create urgency and frequent bathroom trips.
At the same time, the brain may receive false signals that the bladder is full. That’s why some women wake repeatedly at night or experience leakage even when only a small amount of urine is present.
The system isn’t broken—but it is out of sync.
Why Overactive Bladder Happens
There isn’t one single cause. Overactive bladder often develops from a combination of factors.
Neurological causes
Conditions that affect the nervous system can interfere with bladder signaling, including:
Stroke
Multiple sclerosis
Parkinson’s disease
Alzheimer’s disease
Spinal cord conditions or injuries can also disrupt bladder control, since the nerves that regulate urination originate in the lower spine.
Non-neurological causes
Certain foods and drinks can irritate the bladder lining and trigger symptoms, including:
Caffeine
Alcohol
Carbonated beverages
Artificial sweeteners
Spicy or acidic foods
Citrus
Dark chocolate (for some people)
Other contributors may include urinary tract infections, bladder stones, certain medications (such as diuretics), and chronic conditions like diabetes.
Hormonal changes
During menopause, declining estrogen levels can affect bladder and urethral tissue, increasing sensitivity and urgency.
Idiopathic overactive bladder
Sometimes, no clear cause is identified. Even then, treatment can still be very effective.
Why a Bladder Diary Is So Helpful
One of the most useful tools in evaluating overactive bladder is a bladder diary.
This simple log tracks:
Fluid intake
Bathroom visits
Leakage episodes
Nighttime urination
Patterns often emerge. Excess fluid intake, bladder irritants, or nighttime habits may explain symptoms. In other cases, severe symptoms despite minimal intake suggest the need for more advanced treatment.
This information helps guide a personalized and effective care plan.
Treatment Options for Overactive Bladder
Lifestyle adjustments
Treatment often starts with small, meaningful changes:
Reducing bladder irritants
Adjusting fluid timing and intake
Managing underlying medical conditions
Reviewing medications that may contribute to symptoms
Medications
Certain medications help relax the bladder muscle, reducing spasms, urgency, and frequency.
Advanced therapies
When conservative options aren’t enough, additional treatments may help:
Botulinum toxin injections to calm overactive bladder contractions
Nerve stimulation therapies to restore communication between the bladder and brain
These options can provide long-lasting relief for the right patient.
You Don’t Have to Live This Way
Overactive bladder is common.
But it is not something you have to accept.
No one should plan their life around restroom access or feel embarrassed by a medical condition. Effective treatments exist, and seeking care can be life-changing.
Pelvic health is an essential part of overall health. Understanding your symptoms, identifying patterns, and working with a knowledgeable provider can make a profound difference.
If this resonates with you—or someone you care about—know this:
You’re not alone.
And there is help available.
With proper evaluation and individualized care, life does not have to revolve around the nearest bathroom.
If this message resonated with you, feel free to share it with a friend, sister, or mother who may benefit from understanding her body a little better too. For additional guidance, tips, and exercises focused on pelvic health, follow Dr. Nabila Noor on YouTube, Instagram, and TikTok. Prioritizing your pelvic floor today ensures a healthier, stronger, and more resilient body tomorrow.