Understanding Stress Urinary Incontinence: Causes, Symptoms, and Treatment Options
Have you ever laughed, sneezed, or jumped—and noticed a small leak?
If so, you’re not alone. Many women experience this at some point in their lives. But it’s important to know this:
Leakage is common.
But it is not normal.
And it is not something you have to accept—even after childbirth.
What you may be experiencing is stress urinary incontinence, a common but often overlooked pelvic health condition. Understanding what’s happening in your body is the first step toward regaining comfort, confidence, and an active life.
A Common—but Often Unspoken—Condition
Stress urinary incontinence affects roughly one in three women, yet many never talk about it.
Embarrassment, fear, or the belief that leakage is simply “part of being a woman” can keep people from seeking care. Over time, that silence can quietly shrink daily life.
Many women begin to:
Avoid exercise or movement they once enjoyed
Skip social activities
Rely on pads or liners every day
These adjustments may feel small at first—but they can affect both physical and emotional well-being.
I often meet women like Sarah, a 35-year-old mother of two. After delivering large babies and experiencing a difficult delivery with forceps, she noticed leakage during high-impact exercise. At first, she stopped attending classes. Then she stopped exercising altogether.
Friends told her it was normal.
But it didn’t feel right to her.
Once she sought proper evaluation, Sarah learned that stress urinary incontinence is treatable—and that her body wasn’t broken. With the right care, her quality of life improved significantly.
What Is Stress Urinary Incontinence?
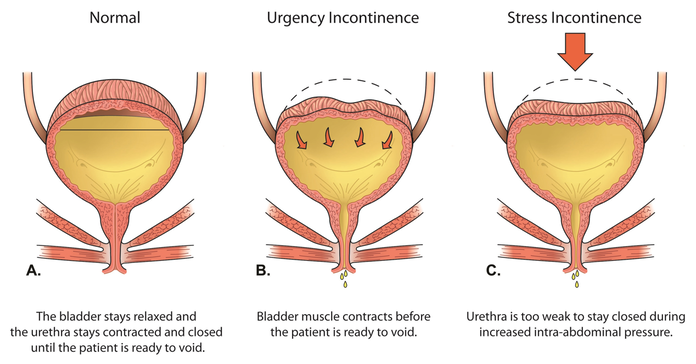
Stress urinary incontinence occurs when urine leaks during activities that increase pressure inside the abdomen—such as laughing, sneezing, coughing, running, or lifting.
Under normal circumstances, the urethra (the tube that carries urine out of the body) stays closed when pressure increases. In stress urinary incontinence, the muscles and connective tissues that support the bladder and urethra have weakened, making it harder to maintain closure.
One way to visualize this is to imagine a garden hose.
When the hose is supported by firm ground, pressure causes it to kink and stop the flow. But when the ground underneath is soft, that same pressure leads to leakage.
The pelvic floor plays a similar supporting role.
Image by Northwestern Medicine
Why Stress Urinary Incontinence Happens
Several factors can weaken pelvic floor support, including:
Pregnancy and childbirth, especially with large babies, prolonged labor, or instrument-assisted deliveries
Chronic constipation or chronic coughing, which increase repeated downward pressure
Excess weight, placing ongoing strain on pelvic tissues
Genetic factors, including connective tissue differences
Prior pelvic surgery or radiation, which can affect muscle or nerve function
Hormonal changes, particularly during menopause, when estrogen levels decline
Stress urinary incontinence can affect women at any age. Some notice symptoms in their twenties; others later in life.
No matter when it starts, help is available.
Non-Surgical Treatment Options
The encouraging news is that many women see significant improvement without surgery. Conservative care is often the first step.
Pelvic Floor Physical Therapy
Targeted pelvic floor exercises can strengthen the muscles that support the bladder and urethra. Technique matters. Many women benefit from working with a pelvic floor physical therapist to ensure the correct muscles are engaged.
With consistency and proper guidance, improvement often follows.
Lifestyle Adjustments
Addressing contributing factors—such as constipation, chronic cough, smoking, or excess weight—can reduce strain on the pelvic floor. For some women in menopause, vaginal estrogen may help improve tissue health and support.
Vaginal Support Devices
Pessaries or urethral support inserts can provide mechanical support and reduce leakage during activity. These devices don’t treat the underlying weakness, but they can significantly improve daily comfort.
Surgical Treatment Options
When conservative treatments are not enough, minimally invasive surgical options may be considered.
Sling Procedures
Sling surgery supports the urethra and helps it remain closed during increases in abdominal pressure. These procedures are typically brief, often performed as outpatient surgery, and have high success rates when used for the right patient.
Bulking Injections
Bulking agents are injected into the urethral walls to improve closure and reduce leakage. This option may be appropriate in select cases.
Other Surgical Approaches
Some women may prefer procedures that use their own tissue rather than synthetic materials. In certain situations, additional surgical techniques may be recommended based on anatomy and prior history.
A thorough evaluation helps determine which option—if any—is most appropriate.
Living With Stress Urinary Incontinence
Stress urinary incontinence should not be accepted as “just how things are.”
With proper diagnosis and individualized care, many women return to the activities they once avoided—without fear or embarrassment.
Seeing a urogynecologist or pelvic floor specialist allows for:
Accurate diagnosis
A personalized treatment plan
Real improvement in daily comfort and confidence
Awareness is powerful. And support is available.
The Bottom Line
Leakage with laughing, sneezing, or exercise is common—but it is not normal.
Stress urinary incontinence is highly treatable, with options ranging from pelvic floor therapy and lifestyle changes to minimally invasive surgery. The right approach depends on your symptoms, your body, and your goals.
If you’re experiencing leakage, you don’t have to endure it quietly.
You’re not alone.
And effective treatment exists.
With the right care, it’s possible to move freely, stay active, and live without the limitations of stress urinary incontinence.
If this message resonated with you, feel free to share it with a friend, sister, or mother who may benefit from understanding her body a little better too. For additional guidance, tips, and exercises focused on pelvic health, follow Dr. Nabila Noor on YouTube, Instagram, and TikTok. Prioritizing your pelvic floor today ensures a healthier, stronger, and more resilient body tomorrow.